COVID Coping

Durante más de medio año, la pandemia de coronavirus (COVID-19) ha cambiado nuestra forma de vivir y de trabajar. Los antiguos alumnos Jonathan Green, Alison Noone, Timothy Leaks, Lakeya Collins y Daniel McCoy se adaptaron rápidamente para hacer frente a retos sin precedentes y satisfacer las necesidades de aquellos a los que sirven.
El liderazgo de Jonathan Green ayuda al personal del hospital a atender a los pacientes durante la pandemia
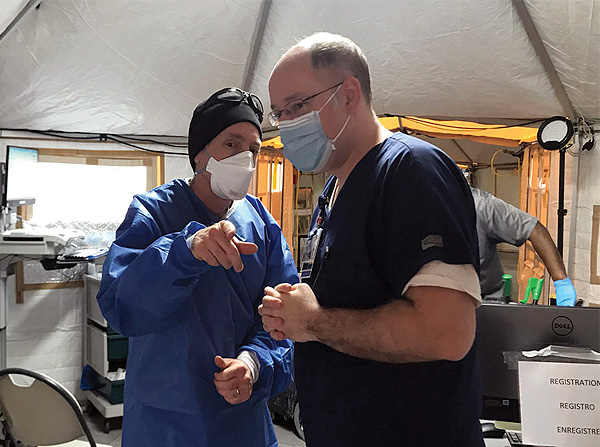
El Hospital Universitario de Newark, Nueva Jersey, fue uno de los hospitales más afectados por los pacientes con COVID-19 en el momento álgido de la pandemia, en la primavera de 2020. Jonathan Green, tres veces graduado del Excelsior College, es el director ejecutivo del servicio de urgencias del Hospital Universitario y, desde marzo, su trabajo consiste en asegurarse de que su personal tenga todo lo necesario para poder atender a los pacientes.
A principios de 2020, el hospital desarrolló protocolos de organización para recibir a los pacientes y hacer pruebas de detección de viajes para el virus, que en ese momento aún no había llegado a Estados Unidos. En marzo, habían montado tiendas de campaña fuera del servicio de urgencias para clasificar a los pacientes e identificar a los que presentaban síntomas. Los hospitales de la ciudad de Nueva York, situada a ocho millas al este de Newark, se enfrentaban a la pandemia con una o dos semanas de antelación, por lo que Green y su personal pudieron prepararse. "Los pacientes que tenían síntomas respiratorios eran evaluados rápidamente por la enfermera de triaje. Los que tenían constantes vitales estables eran atendidos por un médico o una enfermera en una gran carpa fuera del servicio de urgencias para evaluar su estado", dice Green, y añade que si el paciente estaba estable, podía ser dado de alta sin necesidad de entrar en el hospital. Pero como el virus se propagó rápidamente, el personal no pudo detener la afluencia de pacientes y hubo que ingresar en la unidad de cuidados intensivos.
Una de las muchas dificultades a las que se enfrentaron Green y su personal durante el punto álgido de la pandemia, en primavera, fue tranquilizar a las personas que no presentaban síntomas para que siguieran buscando atención médica para lo que les aquejaba.
En el punto álgido de la pandemia, Green afirma que el servicio de urgencias atendió a entre 140 y 150 personas con síntomas al día y que el 75% de ellas dieron positivo en las pruebas del virus. El hospital recibió ayuda del Departamento de Defensa de EE.UU., y un grupo de trabajo de la Reserva del Ejército de EE.UU. ayudó a aumentar el personal médico.
Los hospitales del norte de Nueva Jersey se comunicaron abiertamente entre sí, compartiendo las mejores prácticas, ayudándose mutuamente a coordinar el traslado de los pacientes a los hospitales de campaña y prestando los equipos necesarios. Por ejemplo, los equipos de médicos del Hospital Universitario trabajaron con expertos en enfermedades infecciosas de la Universidad de Rutgers y de todo el país para aprender todo lo posible sobre el COVID-19. Con la ayuda de otros hospitales y del gobierno local y estatal, el Hospital Universitario pudo suministrar al personal respiradores, batas, máscaras, camas de hospital, plexiglás, sábanas de plástico y todo lo necesario para atender a los pacientes. Con estos suministros, Green pudo asegurarse de que su personal tenía los materiales necesarios para mantenerse a salvo y les animó a seguir los protocolos de seguridad, como mantener el distanciamiento social y lavarse las manos.

Una de las muchas dificultades a las que se enfrentaron Green y su personal durante el punto álgido de la pandemia, en primavera, fue tranquilizar a las personas que no presentaban síntomas para que siguieran buscando atención médica para lo que les aquejaba. "La gente con infartos o derrames cerebrales u otros problemas médicos realmente graves tenía mucho miedo de venir aquí", dice. Al final, el hospital descubrió una forma de ayudar a Green a combatir este problema. El hospital organizó actos de divulgación en la comunidad y utilizó las redes sociales para animar a la gente a buscar ayuda. Los medios de comunicación también ayudaron a recordar a la gente la importancia de acudir al médico. El Hospital Universitario puso en marcha las pruebas del virus y designó unidades en el hospital donde Green y su personal atenderían estrictamente a los pacientes con COVID-19 para mantenerlos separados de los pacientes que no tenían COVID-19.
A pesar de las precauciones, Green y varios de sus compañeros acabaron contrayendo el virus. Fue un momento difícil para Green, que quería estar al lado de su personal durante este tiempo en el que Urgencias estaba atendiendo a muchos pacientes. Sin embargo, Green tuvo la suerte de tener sólo síntomas leves y pudo volver al trabajo con relativa rapidez. Una de las razones por las que quería volver al trabajo lo antes posible era porque era duro ver que muchos de sus empleados tenían dificultades para interactuar con los pacientes que estaban tan enfermos de COVID-19. "Eso era una fuente de estrés, y algunos de ellos estaban realmente angustiados por ello", dice Green. El Hospital Universitario buscó la ayuda de dos expertos en salud mental de la Reserva del Ejército de EE.UU. para que apoyaran al personal médico durante este difícil momento.
En septiembre, el número de pacientes que el personal del servicio de urgencias del Hospital Universitario vio con el virus varió cada día. Bajo la dirección de Green, el personal sigue los protocolos de seguridad y se ha adaptado a la nueva normalidad. Se adhieren a la política de enmascaramiento, han ajustado la forma de entregar la comida y han decidido realizar una combinación de reuniones virtuales y en persona para el trabajo administrativo. El principal objetivo de Green sigue siendo apoyar a su personal, los trabajadores de primera línea que atienden a los pacientes. "Me ocupo de las personas que cuidan de los pacientes", dice.
Alison Noone utiliza la tecnología para mantener a los estudiantes comprometidos a distancia
Alison Noone, dos veces graduada de Excelsior, es la subdirectora de vida estudiantil del Ocean County Community College, en la costa de Jersey. Ha experimentado de primera mano los efectos de la pandemia de COVID-19 en las instituciones de enseñanza superior. Aun así, ella y su personal han tomado medidas exitosas para adaptarse a la nueva norma, incluyendo el desarrollo de una aplicación para dispositivos móviles que ayuda a los estudiantes a mantenerse en contacto entre sí y con el colegio comunitario.
Noone lleva casi dos décadas en el Ocean County Community College, comenzando como trabajadora estudiantil en la Oficina de Vida Estudiantil y asumiendo después puestos de creciente responsabilidad. Actualmente se encarga de mantener a los estudiantes comprometidos y de animarles a avanzar en sus estudios.
Desde el brote de COVID-19, el Ocean County Community College se ha vuelto 100% remoto. Nadie puede apreciar que pueda ser difícil para muchos estudiantes la transición al aprendizaje sólo en línea. "Lo siento por los estudiantes que no querían tomar clases en línea. He tomado clases en línea y he tomado clases como estudiante tradicionalmente, cara a cara, y es una transición. Si usted'se ven obligados a ello, entiendo que es difícil de aceptar y es un concepto duro", dice.
Los planes para ofrecer todas las clases, excepto algunos laboratorios de biología, a distancia continuarán al menos hasta el semestre de primavera de 2021. Por lo tanto, la participación de los estudiantes también tendrá lugar en línea. Los estudiantes se relacionan con la universidad virtualmente, a través de Canvas para los cursos, y a través de una aplicación que la Oficina de Vida Estudiantil ha desarrollado junto con la empresa de comunicaciones Ready Education.
Desde el brote de COVID-19, el Ocean County Community College se ha vuelto 100% remoto. Nadie puede apreciar que puede ser difícil para muchos estudiantes la transición al aprendizaje sólo en línea.
Normalmente, la aplicación es sólo una herramienta de apoyo, pero ahora que todo es virtual, se ha convertido en un salvavidas para los estudiantes. "Cada vez que ocurre algo importante o se hace un gran anuncio, tenemos un pico de 1.000 inscripciones en la aplicación al día; tenemos una avalancha de mensajes y preguntas", dice Noone. Los estudiantes han aceptado la funcionalidad de la aplicación, que les permite comunicarse entre sí y con la universidad.

Noone dice que han podido utilizar la aplicación para seguir cuándo y cuántos estudiantes se registran en ella a lo largo del día. Con esta información, han llevado a cabo concursos de trivialidades, han creado clubes virtuales e incluso han organizado noches de cine en las que los estudiantes podían ver una película en sus ordenadores o dispositivos inteligentes y participar en un chat correspondiente con otros en el lado de la pantalla. Con todas las formas creativas en que el departamento de Noone ha utilizado la aplicación, Ready Education les ha reconocido por sus mejores prácticas.
El programa de liderazgo extracurricular que Noone dirige para los estudiantes también ha cambiado a una experiencia más virtual. Normalmente se trata de una serie de tres partes con oradores públicos, Noone ha trabajado para ofrecer los cursos del programa en línea con presentaciones grabadas y enlaces a vídeos de sus colegas de Vida Estudiantil. El programa no cuenta para obtener créditos universitarios, pero es un gran refuerzo para el currículum, dice Noone.
La Oficina de Vida Estudiantil trabaja totalmente a distancia, pero Noone visita el campus con regularidad para gestionar la despensa de alimentos de la universidad. La despensa técnicamente no está abierta durante este tiempo para recoger donaciones, por lo que Noone se ha asociado con un banco de alimentos local para proporcionar cajas de alimentos preparadas a los estudiantes que lo necesitan. Los estudiantes se inscriben por adelantado para reservar una caja de alimentos y luego vienen al campus a recogerla. Las cajas de alimentos se colocan directamente en los maleteros de los coches de los estudiantes para minimizar el contacto social. A los estudiantes que no pueden desplazarse al campus, Noone les envía personalmente tarjetas regalo que la universidad ha comprado en una tienda de comestibles local para que puedan conseguir los suministros que necesitan.
Seguir siendo virtual parece ser la norma para lo que queda de 2020 y Noone se ha comprometido a garantizar que los estudiantes tengan las herramientas y los métodos que necesitan para satisfacer sus necesidades educativas. "Quiero que los estudiantes de Ocean [County Community College] tengan éxito y crean que pueden hacerlo, a pesar de todos los retos que deben superar", afirma.
Timothy Leaks mantiene un barco apretado para mantener a los miembros del servicio seguros y alimentados
Alimentar a 300 militares por comida durante una pandemia puede parecer una tarea sencilla, pero no es tan fácil como parece.
Timothy Leaks, director del comedor del 3er Regimiento de Infantería de los Estados Unidos (La Vieja Guardia) en Arlington, Virginia, se encarga de esta tarea todos los días. Sin embargo, gracias a las orientaciones de los Centros para el Control y la Prevención de Enfermedades (CDC) y del Estado, se asegura de que su personal siga alimentando a los clientes sin correr riesgos.
"Desde que se produjo la COVID-19, tuvimos que modificar y reestructurar básicamente la forma de hacer negocios aquí", dice Leaks. Antes de la pandemia, los miembros del servicio podían comer en la cafetería, pero ahora el lugar funciona como muchos otros restaurantes de Estados Unidos, ofreciendo sólo comidas para llevar y preenvasadas. Los cambios son necesarios para que la cafetería siga funcionando. Leaks dice que cerrar la cafetería no es una opción; es la única instalación de la zona que puede alimentar a los miembros del servicio. Por ello, Leaks y su personal deben asegurarse de que las instalaciones estén completamente limpias o no podrán abrirse para el servicio.
Leaks, graduado en 2019 con una Licenciatura en Artes Liberales, está inscrito en el programa de Maestría en Ciencias en Justicia Penal del Excelsior College. Él y su personal han estado siguiendo los protocolos del CDC, manteniendo el distanciamiento social, usando máscaras y escudos, y usando guantes en todo momento. Leaks se encarga de supervisar a su personal y asegurarse de que se mantiene a salvo. "Me aseguro de que mantenemos la distancia, me aseguro de que nos lavamos las manos como se supone que debemos hacerlo... Me paseo y me aseguro de que todo el mundo hace lo que se supone que debe hacer", dice Leaks. A veces, mantener la distancia social cuando se prepara la comida cerca es difícil. Por ejemplo, suele ser incómodo para el personal cuando la temperatura en la cocina puede alcanzar hasta 120 grados Fahrenheit. Ahora, con la adición de las medidas de seguridad necesarias debido a la pandemia, moverse por la cocina caliente se ha vuelto aún menos agradable.
Él y su personal han seguido los protocolos del CDC, manteniendo el distanciamiento social, usando máscaras y escudos, y usando guantes en todo momento. A Leaks le corresponde vigilar a su personal y asegurarse de que se mantiene a salvo.
Para aliviar la presión sobre el personal de cocina y evitar aún más la contaminación, Leaks organizó al personal en un turno de mañana y otro de tarde para que pudieran entrar y salir del trabajo sin interactuar entre sí. Establecer los turnos de esta manera ha ayudado a minimizar el riesgo de propagación del virus COVID-19. Desgraciadamente, cuando el personal ha enfermado, el trabajo se ha vuelto difícil porque normalmente sólo hay 13 personas asignadas por turno. Por eso, cuando algunas personas han enfermado y han tenido que hacer cuarentena, su ausencia ha hecho que el trabajo sea más estresante para el personal.
Aun así, Leaks y su equipo han salido adelante y han conseguido seguir alimentando a los hambrientos militares que entran por las puertas de la cafetería. A todos los que entran en la cafetería se les comprueba la temperatura y deben llevar una mascarilla en todo momento. El cumplimiento de estas directrices es fundamental para que Leaks pueda gestionar adecuadamente la operación. Leaks y su personal no sólo siguen las directrices de seguridad, sino que también reciben información actualizada sobre el virus por parte del personal médico y sesiones informativas sobre los procedimientos de saneamiento.

Leaks cree que los nuevos procedimientos de seguridad estarán vigentes mucho más allá de los próximos meses. "Incluso cuando el COVID-19 desaparezca, estas son cosas que podría ver en el futuro percibido", dice. Eso le parece bien porque cree que, además de su personal, la gente debería haber tomado desde el principio simples precauciones de seguridad, como lavarse las manos correctamente. El factor de contagio del virus es algo personal para Leaks; tiene un cónyuge de alto riesgo y un hijo pequeño en casa, así que sabe lo importante que es mantener los protocolos de seguridad. De hecho, en cuanto Leaks vuelve a casa del trabajo, va directamente al garaje para cambiarse de ropa, lavarse y limpiar su coche. Cuando se trata de su familia, no quiere correr ningún riesgo.
Además, Leaks está agradecido por el apoyo de su familia y también por un terapeuta conductual con el que puede hablar cuando las cosas se ponen demasiado estresantes. A menudo le preocupa que los clientes se expongan al COVID-19 y le inquieta la falta de conocimientos que rodea al virus. A pesar de estas preocupaciones, Leaks mantiene el orden para su personal y les proporciona la información y los suministros que necesitan para hacer bien su trabajo. Y si su personal también está estresado y preocupado, tiene la oportunidad de ponerse en contacto con los servicios profesionales que el centro le ha proporcionado. Como veterano de 20 años, Leaks está acostumbrado a hablar con alguien y se alegra de que haya proveedores disponibles, que ofrecen apoyo a los trabajadores de primera línea como él.
Con la supervisión de Leaks en el comedor, los militares de la zona de Arlington tienen garantizada una comida -o tres- cada día. Al cumplir las normas, Leaks mantiene a su personal y a sus clientes a salvo. Como resultado, al seguir también sus protocolos personales y mantener una mente sana, está mejor preparado para dirigir a su equipo para que pueda proporcionar comida y una sensación de normalidad durante un momento tan crítico.
Lakeya Collins toma medidas adicionales para cuidar a los residentes de la residencia de ancianos
Según un estudio publicado en USA Today, los residentes de las residencias de ancianos representan casi el 40 por ciento de las muertes por COVID-19 del país. Sorprendentemente, la residencia de ancianos en la que trabaja Lakeya Collins no vio ningún caso del virus hasta septiembre de 2020, en parte gracias a la dedicación de Collins para mantener la seguridad de los residentes.
Collins, una graduada de 2018 que obtuvo un grado asociado en enfermería, ha estado trabajando para ayudar a mantener la baja tasa de infección por el virus en The Place at Dean's Bridge, un centro de enfermería especializada en Augusta, Georgia. A mediados de septiembre, el hogar de ancianos tenía 16 casos confirmados, pero durante más de seis meses antes de eso, el hogar de ancianos tenía cero casos. Se trata de una hazaña notable, ya que en el condado de Richmond, donde se encuentra Augusta, había aproximadamente 785 casos de COVID-19 a finales de junio y el número de personas diagnosticadas con COVID había aumentado un 8,4% desde entonces. El 5 de septiembre, había 280.000 casos en Georgia; 6.634 de ellos estaban en el condado de Richmond.
En un principio, The Place at Dean's Bridge consiguió mantener las tasas de infección a cero gracias a la dedicación de los empleados. Al inicio de la propagación del virus, Collins se unió a un grupo de trabajo especial de COVID-19 para ayudar a implementar y mantener los procedimientos de seguridad para que los residentes del centro permanecieran a salvo de la infección. El centro ha seguido las directrices de los Centros para el Control y la Prevención de Enfermedades (CDC) y ha mantenido estrictas normas de distanciamiento social para evitar el contagio entre el personal. Los residentes se someten a pruebas de detección del virus dos veces por semana para controlar su propagación.
Como no se permiten las visitas, para que el centro pueda mantener el distanciamiento social, Collins se ha encargado de asegurarse de que sus pacientes tengan contacto con sus seres queridos.
Como miembro del grupo de trabajo, Collins se encarga de que se comprueben las constantes vitales de los residentes, pero dice que sólo pueden evaluar a los residentes que han dado negativo en la prueba COVID-19. También toma medidas adicionales para cuidar el bienestar emocional de los pacientes. Dado que no se permiten las visitas, para que el centro pueda mantener el distanciamiento social, Collins se ha encargado de asegurarse de que sus pacientes tengan contacto con sus seres queridos. Prestándoles su teléfono móvil personal, pueden hacer llamadas FaceTime con sus familiares. También intenta disuadir a los residentes de que vean las noticias relacionadas con el COVID-19 porque no quiere que se alteren por la información negativa. Mantener una actitud positiva con los residentes es difícil, pero Collins intenta añadir algo de felicidad al día de todos. "Puede que vaya a comprarles nuggets de pollo, algo que les haga seguir adelante, que les haga sonreír", dice Collins. También pone música y lee escrituras a muchos de los residentes, lo que les hace ver el lado positivo.
Hay que reconocer que Collins estaba nerviosa e incluso paranoica en los primeros meses de la pandemia, comprobando constantemente su temperatura y asegurándose de no entrar en contacto con otras personas. Ver en las noticias locales y nacionales a personas con respiradores y en unidades de cuidados intensivos fue duro, lo que hizo que su trabajo fuera estresante. Con el tiempo, dice que se ha acostumbrado a ello. "Es como todo en la enfermería; usted se acostumbra a ello. usted hace lo que usted'se supone que debe hacer", dice. Ahora que varios residentes están infectados, Collins se asegura aún más de mantener las medidas de seguridad adecuadas, incluyendo el lavado de manos antes de ir a casa. Aunque toma precauciones, no quiere contagiar inadvertidamente el virus a su hijo de 10 años. "Ese es mi mayor temor, pero hacemos todo lo posible para asegurarnos de que nuestra vida diaria sea segura", dice.
Collins cree que ha hecho un buen trabajo cuidando a los residentes y se esfuerza por seguir las directrices de los CDC y de su centro. Durante esta pandemia, quiere que la gente entienda lo que realmente ocurre en los hospitales e instalaciones como The Place at Dean's Bridge para mantener a la gente a salvo, y que preste atención al virus. Dice: "Sólo quiero que la gente se lo tome más en serio [el COVID-19] para que podamos superar esta parte de aumento de las cifras, podamos conseguir una vacuna y la gente pueda seguir con su vida en un espacio seguro en medio de ella".
El funcionario electo Daniel McCoy mantiene el contacto con el público para mantener la seguridad de las personas
Como ejecutivo del condado, el ex alumno de 2009 Daniel McCoy está dirigiendo el condado de Albany, en el noreste del estado de Nueva York, a través de la pandemia de COVID-19. Su trabajo de proporcionar a la gente los hechos y hacerles saber qué recursos están disponibles a través de la Oficina del Ejecutivo del Condado ha resultado difícil durante este tiempo de distanciamiento social. Sin embargo, a pesar de los desafíos, ha sido capaz de mantenerse en contacto con el público.
McCoy no es ajeno al COVID-19 y sabe cómo puede afectar a las personas. Se sometió a una prueba de anticuerpos en mayo que reveló que tenía anticuerpos contra el coronavirus, lo que significa que había contraído el virus anteriormente. Los médicos estiman que McCoy probablemente lo tuvo en algún momento del invierno 2019-2020. En un artículo para el Times Union [Albany, Nueva York] publicado el 3 de agosto de 2020, dijo: "Fue aterrador porque no sabía a qué me enfrentaba en ese momento, pero sabía que estaba realmente enfermo. Eso no significa que no pueda volver a tenerla. Sólo significa que la tuve una vez y la superé. Así que soy prudente".
Su cautela está ayudando a mantener a los demás seguros e informados. Desde el mes de marzo, McCoy ha estado celebrando sesiones informativas diarias para proporcionar información sobre seguridad al público. Durante estas sesiones informativas, que se muestran en Facebook, se publican en la página web de la oficina y son cubiertas por los medios de comunicación locales, McCoy ofrece regularmente actualizaciones y transmite información sobre el distanciamiento social, el uso de una mascarilla, la buena higiene de las manos y el mantenimiento de los gérmenes al toser en el codo. "Intentamos ser proactivos. No intentamos asustar a nadie. Sólo tratamos de decir, está aquí, ha estado aquí, [y] tenemos que mantener la calma, pero usted tiene que estar preparado", dijo McCoy.
Para ayudar en cuestiones relacionadas con la seguridad, la oficina ejecutiva también comenzó a proporcionar vídeos sobre proyectos de artesanía y otras actividades para realizar con los niños, así como a dar consejos para mantener la salud mental. McCoy ordenó al Departamento de Salud Mental del Condado de Albany que estableciera una línea de apoyo COVID-19 para que las personas de la comunidad que sufren estrés, ansiedad o depresión puedan llamar los siete días de la semana.
El COVID-19 ha traído muchos días de prueba, y McCoy dice que el 28 de marzo fue un día particularmente oscuro. Tuvo que anunciar la primera muerte por el virus en el condado de Albany. "Para mí, como ejecutivo del condado, es un duro golpe para usted . Es importante recordar que todas y cada una de las muertes representan a una familia o a unos seres queridos que acaban de perder a alguien extremadamente importante para ellos", dice. El 28 de marzo también fue difícil porque McCoy y su personal se dieron cuenta de que la pandemia no había hecho más que empezar y que había un duro camino por delante.
Ese duro camino por delante es algo que mantiene a McCoy despierto por la noche.
Hasta el 12 de septiembre de 2020, ha habido 2.859 casos y 134 muertes por COVID-19 en el condado de Albany. Aunque cualquier número es una mala cifra, la tasa de infección del condado de Albany es mucho menor que la de otras áreas metropolitanas del estado. Por ejemplo, la ciudad de Nueva York ha notificado 242.000 casos, el condado de Erie (área de Buffalo) ha notificado 10.444, el condado de Monroe (área de Rochester) ha notificado 5.649 y el condado de Onondaga (área de Syracuse) ha notificado 4.023. Mantener las cifras del condado de Albany comparativamente bajas ha sido la principal misión de McCoy.
"Mi trabajo como líder ha sido proporcionar ese liderazgo que la comunidad necesita, informar a los miembros de lo que está sucediendo y darles la ayuda que requieren". - Daniel McCoy
"Mi trabajo como líder ha sido proporcionar ese liderazgo que la comunidad necesita, informar a los miembros de lo que está ocurriendo y darles la ayuda que necesitan", dice McCoy. En febrero, colaboró estrechamente con la Guardia Nacional para ayudar a entregar cajas de alimentos a las personas en cuarentena. Siendo él mismo miembro de la Guardia Nacional, McCoy ha utilizado sus experiencias militares pasadas para informar su enfoque de liderazgo durante esta pandemia. Dice que usted debe actuar con rapidez en tiempos de crisis, algo que aprendió cuando estaba alistado.
Con el liderazgo de McCoy, el condado de Albany tomó medidas para garantizar la equidad sanitaria. El condado de Albany se convirtió en el primer condado de Nueva York en establecer sitios de pruebas móviles para las personas que no podían viajar para hacerse la prueba del virus (y la iniciativa se extendió a los condados vecinos). También se asoció con la Liga Atlética de la Policía de Albany, que crea asociaciones entre los jóvenes, la policía y la comunidad a través de programas de colaboración, y con AT&T para lanzar un reto en Instagram que animaba a los adolescentes a publicar vídeos y fotos que mostraran cómo se mantenían seguros.

Mantener a todo el mundo a salvo no ha sido fácil; después de una gran fiesta para celebrar el 4 de julio, el condado de Albany vio un aumento en el número de casos de COVID-19. Esto hizo que McCoy utilizara el tiempo durante sus sesiones informativas diarias sobre COVID-19 para animar al público a seguir las precauciones de seguridad. Y, durante este tiempo crítico, las oficinas del condado de Albany, incluida la de McCoy, nunca cerraron. McCoy dice que quiere asegurarse de que está disponible para responder a las preguntas que ha recibido del público en el sitio web del condado o en Facebook.
Para McCoy, mantenerse en contacto con los residentes del condado es la mejor manera de mantener a la gente a salvo. Continuará con sus sesiones informativas diarias y sus constantes actualizaciones en las redes sociales para mantener a la gente informada sobre la nueva información de salud y seguridad, y trabajará todo lo que pueda para mantener las tasas de infección por COVID-19 del condado de Albany relativamente bajas.







